
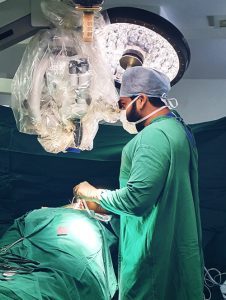
 The surgical Microscope has revolutionized the practice of spine surgery. Magnification, Stereoscopic View and Illumination has contributed to the evolution of Minimally Invasive approaches, possibly leading to better surgical outcomes.
The surgical Microscope has revolutionized the practice of spine surgery. Magnification, Stereoscopic View and Illumination has contributed to the evolution of Minimally Invasive approaches, possibly leading to better surgical outcomes.
Magnification from the microscope can allow the surgeon to appreciate greater anatomical detail, particularly during the execution of finer dissection techniques as is required with intradural spinal lesions.
Microsurgery with the operating microscope has lead to small incisions, less muscle dissection and trauma. Studies comparing microdiscectomy to standard discectomy has shown Decreased Length Of Hospital Stay,
Lower Analgesic Requirements and Early Return To Work when compared to standard discectomy patients.
The microscope in Cervical spine approaches can greatly help the surgeon to avoid complications during decompression of the spinal cord and nerve roots through better illumination and magnification.
The benefits of using an operating Microscope include –
- Smaller incision
- Little or no muscle cutting
- Less bleeding during surgery
- Shorter hospital stays
- Smaller risk of infection
- Less pain after surgery
- Faster recovery
- Less rehabilitation is needed
- Less scarring
The spine surgery robot is a tool that facilitates the surgeon’s pre-operative plan.
Much like a pilot formulates a pre-flight plan depending on the weather, route, payload, and fuel level, a surgeon formulates a pre-surgical plan in a virtual environment based on the anatomy, bone quality, and desired correction of deformity. That plan is done on a pre-operative CT scan and once complete, the plan is loaded into the robot’s computer.
During surgery, the robot facilitates the plan by pointing out the site for screw insertion, and the location and extent of bone removal.
The robot is passive in that it does not do the surgery—the surgeon still performs the surgery much like the pilot of a plane still flies the plane. The robot’s role is to help the surgeon be more efficient and precise.
The initiation of robotic spine surgery technology was 18 years ago and has evolved through 3 generations, with substantial improvements along the way.
The use of spine surgery robots is now just becoming mainstream. There are multiple commercial robots available. Within the next 5 years the use of a robot to perform complex spine surgery will be the standard of care.
Robotic spine surgery can be performed in a traditional operating room setting in a hospital. The robot can facilitate less invasive approaches, so surgery can be accomplished as an outpatient procedure. This technology also facilitates even the most complex surgery that needs to be performed in an inpatient setting.
Robotic spine surgery shortens operating time. The robot does not make a bad surgeon good, it makes a good surgeon more efficient and precise.
Any procedure where instrumentation (eg, screws) or implants need to be applied to the spine can be achieved using robotic spine technology. Also, robotic spine surgery may be used for any procedures where bone needs to be removed or cut from the spine.
Robotic spine surgery technology is most beneficial for complex revision surgery, where the anatomy may be distorted due to previous surgery. It’s also beneficial for deformity surgery where you have to predict the final shape of the spine and place screws in optimized locations to obtain the needed correction.
When patients hear “robotic spine surgery,” many assume that the robot is actually performing the surgery—but that’s not true. The surgeon still does the surgery. The robot is not a surgeon but rather a tool to assist the precision and efficiency of the surgery. The technology is very safe.
The benefits of robotic spine surgery include increased efficiency and accuracy. That translates into less time under anesthesia for the patient and less economic cost to the system.







